If the payer requires that an independent medical exam (IME) be conducted before it responds to an MTG variance or MTG special services prior authorization request (PAR), the payer must notify the claimant, claimant’s attorney (if applicable) and the requesting health care provider within five days of the PAR’s submission date. When the IME Requested Notification is timely sent to the provider in OnBoard, the timeframe for response will automatically be extended from 15 days to 30 days.
To submit the IME Requested Notification, select that specific PAR ID link in the dashboard.
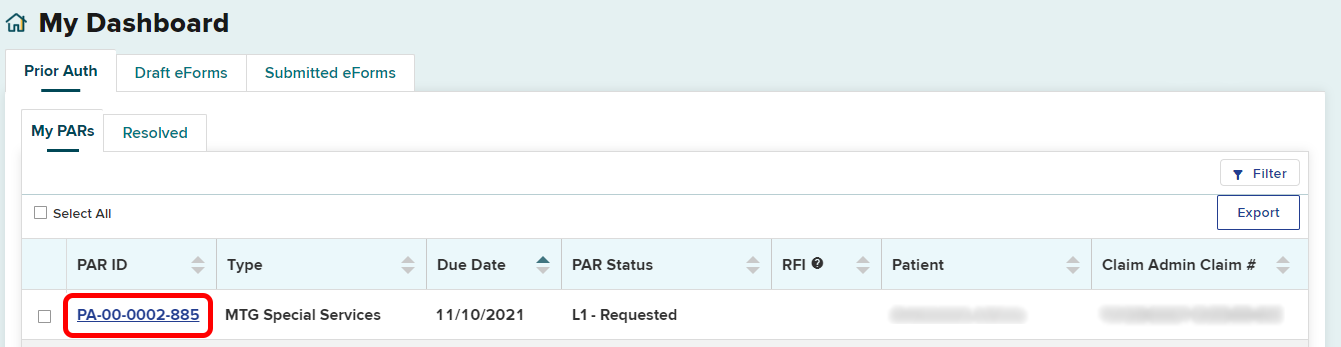
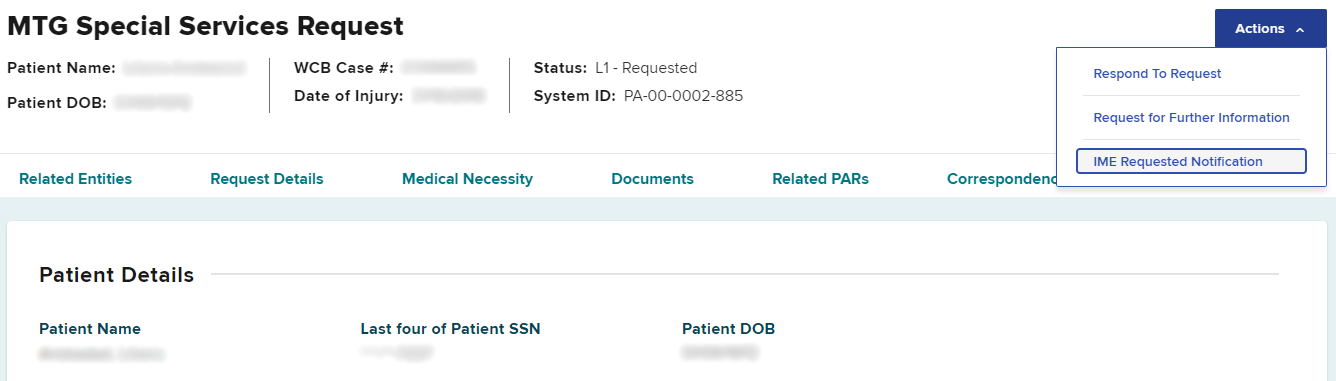
On the PAR details page, select the Actions dropdown button on the top right and select IME Requested Notification.
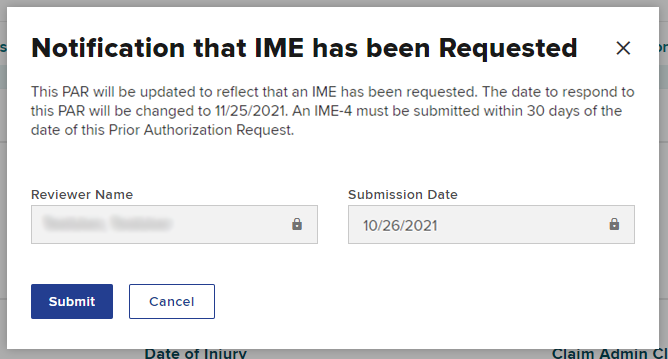
A pop up will appear to submit the notification that an IME has been requested. Review the information regarding updated timeframes and the requirement that the IME-4 must be submitted within 30 days. Select Submit.
At the bottom of your dashboard, a confirmation will appear confirming that the response has been submitted and clarifying the new due date for a payer response.
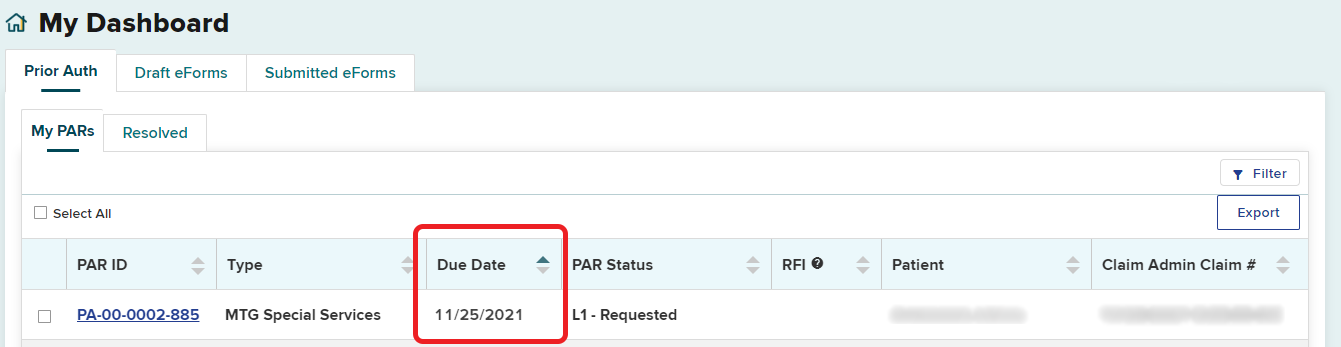
The date in the Due Date column will be extended by 15 days, allowing 30 days for an IME to be conducted and for you to respond.
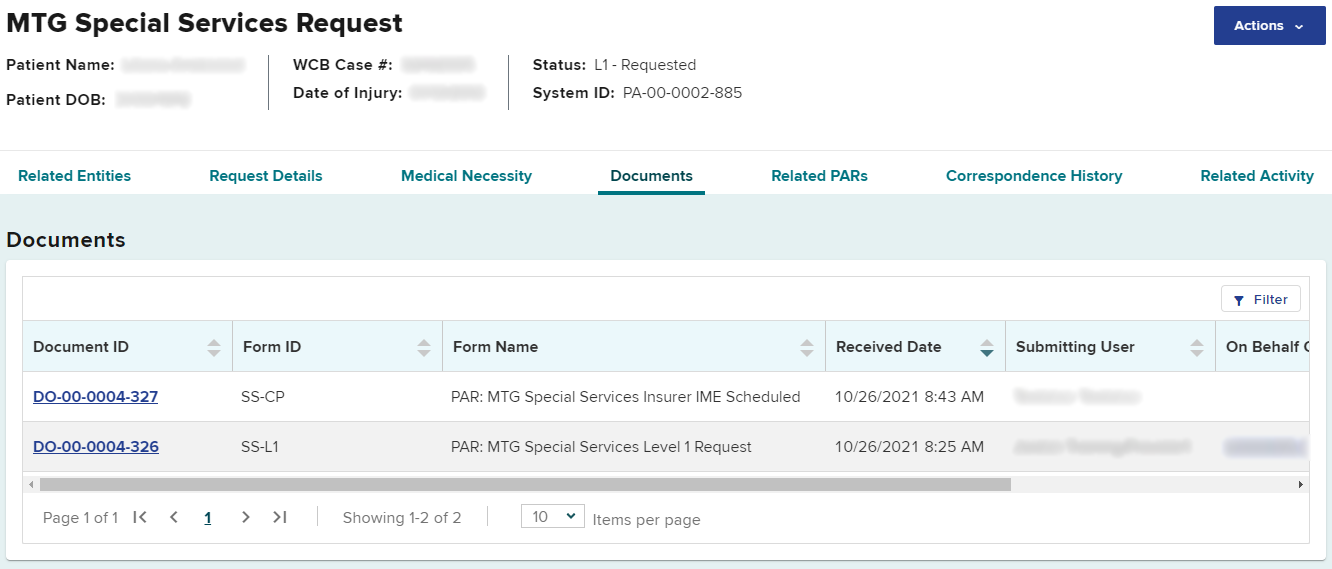
When an IME request notification is sent, a document will be generated, and a link will be added to the Documents section on the PAR details page.
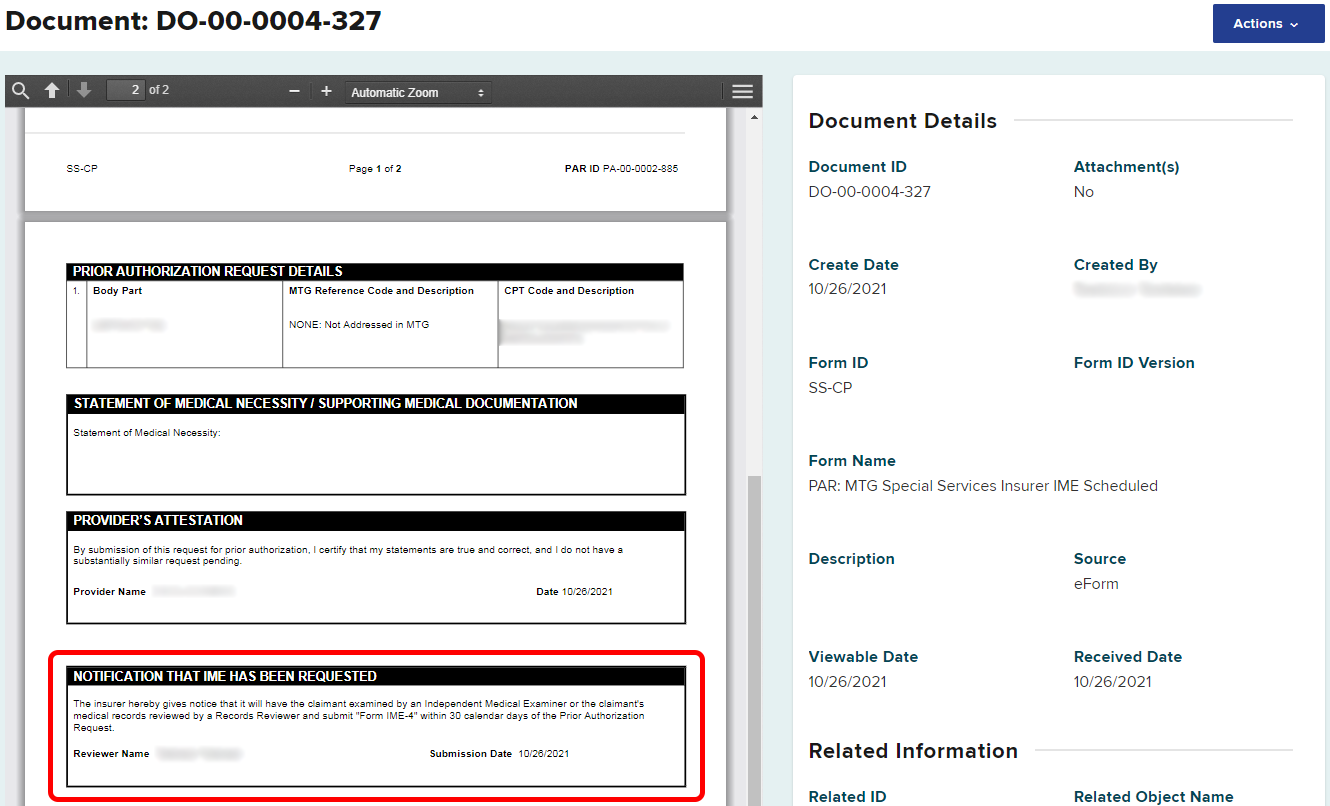
Select the Document ID link to view the full document, which contains all PAR details, including an updated section with the IME notification.
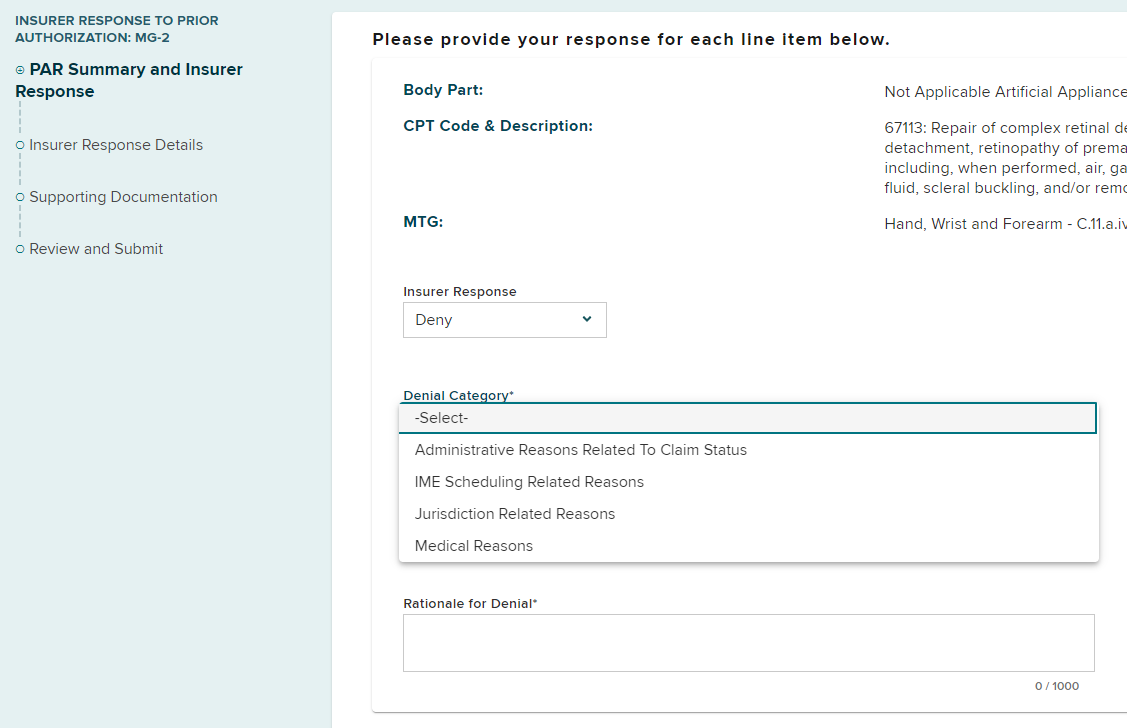
PAR denial for IME scheduling related issues
If the PAR type is MTG Variance or MTG Special Services and you have sent an IME Requested Notification in OnBoard, or the PAR type is a Non-MTG Under $1,000, an IME Scheduling Related Reasons option will be available in the Denial Category drop-down for situations where the claimant fails to appear for the IME or initiates a reschedule outside your timeframe to respond to the PAR. The injured worker or their attorney may submit a Request for Further Action to have the denial reviewed by the Board or the provider may submit another request with updated documentation.